Pain
Diagnosing a Herniated Disc(s)

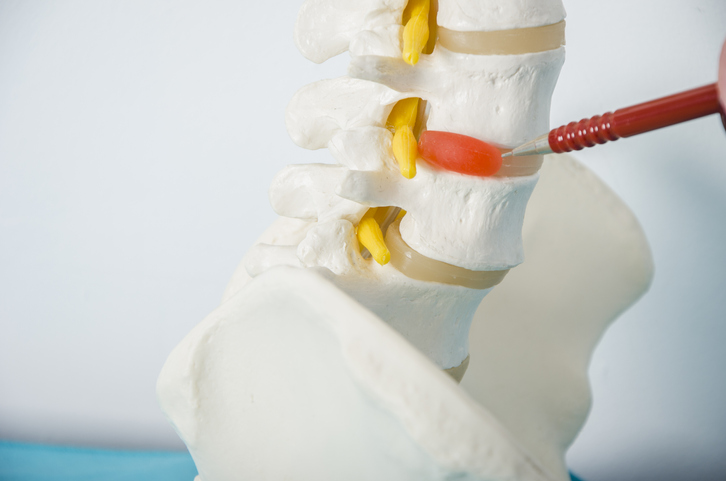
What is a herniated disc?
Spinal discs are the rubbery cushions that act as shock absorbers between individual spinal vertebrae. As a disc naturally degenerates with age, the soft, jelly-like center of the disc (nucleus) can dehydrate, deteriorate, slip, collapse, protrude, rupture or tear through the tougher, rubbery exterior (annulus). In addition to natural degeneration of the spinal discs, other causes of herniated discs include trauma, a heavy blow to the back, or twisting or turning while lifting a heavy item.
A herniated disc can occur at any point of the spine, but cervical (neck) and lumbar (lower back) spinal discs are most commonly affected. The damaged disc(s) can irritate nearby nerves and cause pain, weakness, numbness, or radiating pain in the legs or arms. The pain typically worsens during physical activity and lessens during rest.
Diagnosing herniated discs
A health care professional should be consulted if a herniated disc is suspected. A thorough medical history, physical exam, and imaging tests are part of the diagnostic process.
Medical history
A medical history typically includes questions similar to the following:
- When and how did the pain begin?
- Where is the pain located?
- What does the pain feel like?
- What helps to ease the pain, and what causes it to worsen?
- Are other pre-existing health conditions present?
- Is there a history of back issues?
- What is the family medical history?
- Is depression or anxiety present?
Physical exam
A physical exam is typically conducted before diagnostic tests are ordered. During the exam, a health care professional will
- determine levels and areas of pain with the individual lying on their back while lifting or moving their legs in specific positions.
- determine the level of tenderness in the back.
- check reflexes of the knees and ankles.
- determine the amount of strength in the legs.
- observe bending and stretching abilities.
- observe walking ability.
- check the ability to feel light touch or vibration.
Imaging tests
- X-rays
X-rays are used to determine if the pain is caused by a fracture or tumor and to eliminate the possibility of other back conditions. X-rays are typically not used independently of other tests to diagnose a herniated disc. - Myelogram
A myelogram is a type of X-ray that is performed after a dye is injected into the spinal fluid. It can determine the location of any pressure on the spinal cord. Although this is an invasive test, it can determine the size and location of a herniation. - CT scan (CAT)
A CT scan uses X-ray technology to create images of the spinal cord and surrounding structures from varying angles. - MRI (magnetic resonance imaging)
An MRI uses radio waves, a magnetic field, and a computer to create detailed images of the spinal cord. MRI images provide a detailed look inside a herniated disc to show the precise location of the herniation and which nerves are involved. - Electromyogram (EMG)
An electromyogram involves the insertion of a needle electrode into a muscle to record electrical activity. This test detects the small amount of electricity that muscle cells make when stimulated, which helps determine if nerves are damaged or compressed. - Nerve conduction studies (NCS)
Nerve conduction studies use slight electrical impulses to stimulate the nerves. They are oftentimes done in conjunction with an EMG. Electrodes are placed on different areas of the body to determine the travel time of nerve impulses. This test can help identify the extent of nerve damage.