Pain
Aging Effects on the Spine
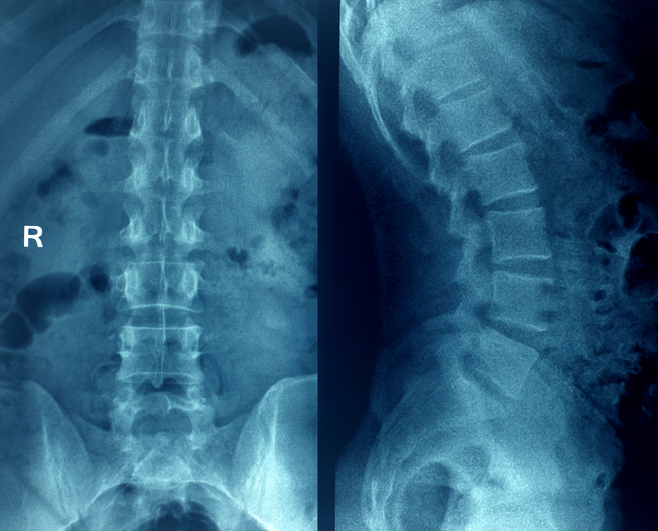
The spine of an average adult consists of 24 vertebrae (bones) that connect with facet joints. Discs are jelly-like cushions separating the bones of the spine (vertebrae). Ligaments stabilize the spine. During the aging process, discs lose fluid and become thinner. The vertebrae lose mineral content, resulting in thinner bones. The spinal column becomes compressed, resulting in curvature. Bone spurs may also develop on the vertebrae.
The sacrum is the bottom of the spine. The cervical spine (neck) has seven bones, the thoracic spine (chest) has 12 bones, and the lumbar spine (lower back) has five bones. The spinal column is composed of the vertebrae, ligaments, tendons, muscles, facet joints, and discs.
Aging and the spine
The spine begins to age in the 20s and 30s and continues to age throughout life. The natural process of aging causes the loss of bone mass or density. The bones lose calcium and other important minerals. Spinal stenosis, spondylolisthesis, and osteoarthritis are the three most common reasons for back pain after the age of 50.
Spinal stenosis
Spinal stenosis is a narrowing of the spinal canal. It occurs when the bony openings within the spine (foramina) begin to narrow, placing pressure on the nerves traveling throughout the spine. This reduced nerve space can occur within the spinal cord or where the spinal nerves exit the spinal canal.
Spondylolisthesis
Spondylolisthesis is a medical condition that primarily affects the lower back (lumbar spine); however, it can also occur in the mid to upper back (thoracic spine) or neck (cervical spine). Spondylolisthesis occurs when a vertebra slips forward (anterolisthesis) or backward (retrolisthesis) onto the vertebra underneath it, which may lead to nerve compression.
Osteoarthritis
Osteoarthritis (OA) is a joint condition that involves the gradual breakdown of cartilage in one or more joints. When the protective cushioning of cartilage deteriorates, the bones in the joint eventually rub together, causing inflammation and pain. Because OA is typically caused by normal wear and tear, the risk of developing osteoarthritis increases with age. The condition develops gradually and worsens over time.
Warning signs
A health care professional or spine specialist should be consulted for the following:
- Progressive weakness
- Poor balance
- Bowel or bladder changes
- Clumsiness
- Pain persisting more than a few months