Pain
Conventional Medical Treatments for Lymphedema
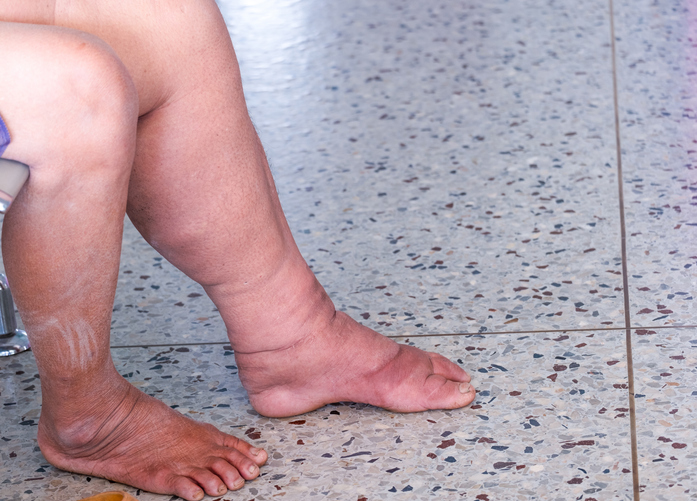
What is lymphedema?
The lymphatic system moves a colorless, watery fluid (lymph) throughout the body to help filter waste and fight off pathogens. Lymphedema develops when the lymphatic system is unable to adequately drain this fluid. Because it is not being properly drained, the fluid accumulates in the surrounding soft tissues, causing swelling and various other symptoms. Lymphedema can occur anywhere in the body but most commonly occurs in the arms and legs.
Conventional treatments for lymphedema
While there is no cure for lymphedema, it can be managed with early diagnosis and diligent care of the affected area(s). Conventional treatments include medications, compression, and therapies.
Medications
Medication treatment for lymphedema is limited but may include ketoprofen, topical medications, or prophylactic antibiotics.
- Ketoprofen is a nonsteroidal anti-inflammatory drug (NSAID) similar to ibuprofen. It may help the symptoms of lymphedema and increase the skin’s elasticity. It may also help reduce the recurrence of infections.
- Topical medications, such as moisturizers, urea, and salicylic acid, may help improve skin damage.
- Prophylactic antibiotics, such as penicillin or erythromycin, can help prevent recurrent infections.
Compression
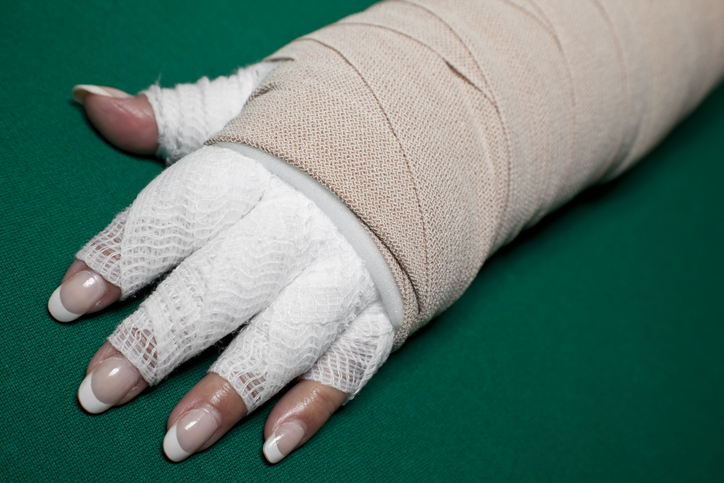
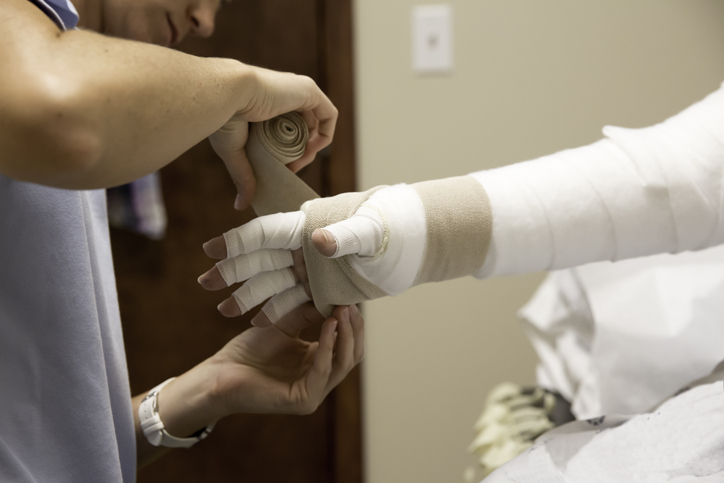
Compression treatment is often helpful. Types of compression devices include bandages, arm pumps, and compression garments.
- Bandages
Wearing a customized elastic bandage or compression sleeve can help prevent fluid build-up. - Arm pump
Using an arm pump can encourage the flow of fluid in lymphatic vessels. - Compression garments
Wearing compression garments, such as long sleeves or stockings made to compress an arm or leg, improves the flow of lymph fluid. Wearing a compression garment during physical activity makes it even more effective. Obtaining a correct fit for a compression garment is important. It should be professionally fit or custom-made if possible.
Physical and occupational therapy
Physical therapy and occupational therapy can both be used to manage symptoms of lymphedema. Working with therapists can help:
- lessen swelling of affected limb(s) or area(s).
- improve skin texture.
- increase flexibility of the skin and joints.
- reduce risk of infections by promoting proper skin care.
- help improve overall mobility.
Complete decongestive therapy
Complete decongestive therapy (CDT) combines therapies with lifestyle changes. CDT typically includes a combination of skin care, manual massage, external pressure, and isotonic exercise. This type of therapy may not be recommended for those with high blood pressure, diabetes, paralysis, blood clots, or acute infections.
Surgery
Surgical intervention is usually reserved for advanced lymphedema. Surgical options include liposuction, lymphovenous bypass, lymphovenous transplant, and skin grafts.
- Liposuction
Excess lymph fluid stored in surrounding tissues can cause inflammation and encourage the growth of fat stem cells. Liposuction removes excess fat tissue generated from lymphedema. This is usually an outpatient procedure. - Lymphovenous bypass
A lymphovenous bypass uses microsurgical techniques to bypass damaged nodes and connecting channels. This is usually an outpatient procedure. - Lymphovenous transplant
A lymphovenous transplant involves transplanting healthy lymph nodes to an area affected by lymphedema; this procedure aims to “rewire” the lymphatic system. A lymphovenous transplant is usually an inpatient procedure, involving a few days for recovery. - Skin grafts
A skin graft involves removing damaged skin and replacing it with healthy skin.