Pain
Progression and Potential Complications of Diabetic Neuropathy
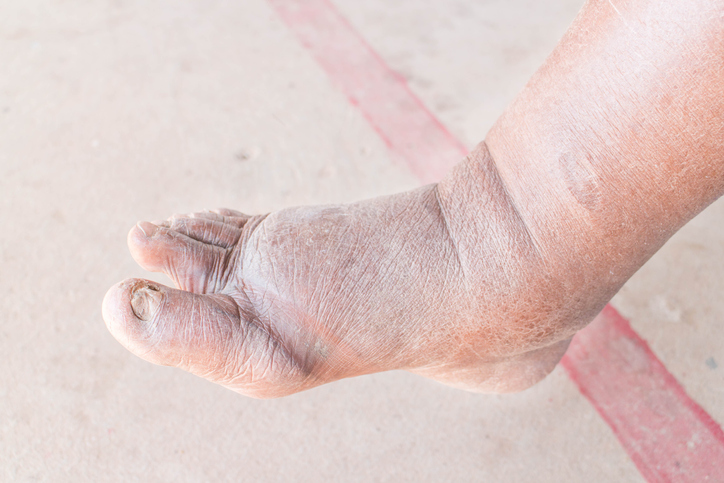
Diabetic neuropathy affects approximately 50% of individuals with diabetes. It develops from long-term elevated blood glucose levels that gradually cause nerve damage.
Diabetic neuropathy is categorized into four main types: peripheral, autonomic, proximal and focal. Symptoms vary depending on the type of diabetic neuropathy and the affected area. Common symptoms include pain and numbness in the legs and feet that may spread to the arms and hands. Issues with the digestive system, blood vessels, heart, or urinary tract may also develop.
Progression of diabetic neuropathy
Untreated diabetic neuropathy follows a natural course of progression that involves nerve degeneration and severe damage. Although there is no known cure for diabetic neuropathy, medical treatments can help slow or prevent progression, relieve pain, manage complications, and restore function. Managing type 1 or type 2 diabetes with proper medical care, blood sugar monitoring, blood pressure control, and a healthy lifestyle is critical in preventing or slowing the progression of diabetic neuropathy.
Potential complications associated with diabetic neuropathy
Potential complications associated with diabetic neuropathy range from moderate to severe. They include, but are not limited to, the following:
- Unawareness of low blood sugar levels
Shakiness, sweating, and an increased heartbeat are symptoms of blood sugar levels falling below 70 milligrams per deciliter (mg/dL). An individual with autonomic diabetic neuropathy may not be aware of these warning signs. - Sudden drop in blood pressure
The body may not be able to adjust blood pressure due to damage to nerves that control blood flow. A sharp drop in blood pressure may occur when standing, which can lead to fainting or dizziness. - Amputation of a toe, foot or leg
A common symptom of diabetic neuropathy is loss of sensation in the feet. Cuts may not be felt and can lead to sores or ulcers. If not treated, this could cause severe infection in the bone or cause tissue death. If this occurs, amputation of the affected area (e.g., toe, foot, or lower leg) may be required. - Urinary tract infections or urinary incontinence
Damage to the nerves in the bladder may cause an inability to fully empty the bladder. This can lead to a build-up of bacteria in the bladder and kidneys, which can cause infections. Nerve damage may also result in the inability to feel the need to urinate or to control muscles that release urine, causing urinary incontinence. - Digestive system issues
Nerve damage in the digestive tract can cause diarrhea or constipation. Gastroparesis (a condition in which the stomach empties too slowly) can also develop, causing bloating and indigestion. - Bodily injury
Because diabetic neuropathy often affects sensory nerves, hot and cold sensations may be experienced differently. For example, a cup of warm coffee may feel extremely hot or scalding water may feel slightly warm. Frostbite or burns may occur due to these changes in temperature perception. Nerve damage may also result in a person not feeling an injury, which could lead to infection or further injury. - Temperature regulation
Nerve damage can affect the sweat glands, causing increased or decreased sweating. This can disrupt the body’s ability to regulate temperature. - Sexual dysfunction
Autonomic neuropathy may affect the nerves of sex organs. Women may experience vaginal dryness and lack of arousal, whereas men may experience erectile dysfunction. - Fall risk
Numbness in the feet is a common symptom of diabetic neuropathy. It may cause difficulties with walking, such as an unsteady gait or balance issues. Muscle weakness may also affect the ankle and gait. These symptoms increase the likelihood of falling. - Hammertoe
Hammertoe is a deformity in which one of the three toes between the big toe and little toe becomes contorted at the joint due to weakened muscles from nerve damage. - Sleep issues
Symptoms of diabetic neuropathy often worsen at night, which can affect sleep. Bed covers may feel heavy, making it difficult to fall asleep.