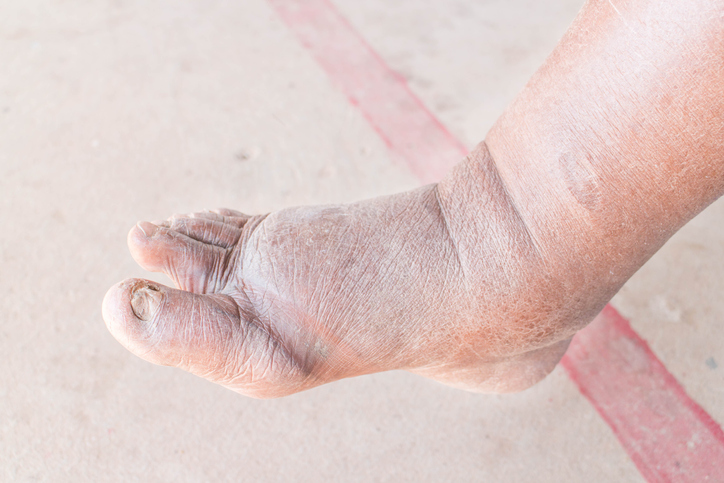
Pain
What is Diabetic Neuropathy?
Diabetic neuropathy affects approximately 50% of individuals with diabetes. It develops from long-term elevated blood glucose levels that gradually cause nerve damage. Managing type 1 or type 2 diabetes with proper medical care, blood sugar monitoring, and a healthy lifestyle is critical in preventing or slowing the progression of diabetic neuropathy.
Types
Diabetic neuropathy is categorized into four main types: peripheral, autonomic, proximal and focal. A person can have one or multiple types of diabetic neuropathy.
Symptoms
Symptoms of diabetic neuropathy range from numbness and pain in the feet or legs to issues with the digestive system, blood vessels, heart, or urinary tract. Symptoms typically develop gradually and range from mild to debilitating. Although symptoms vary depending on the type of diabetic neuropathy and the affected area, common symptoms include the following:
- Numbness or pain in the hands, feet or legs
- Burning sensations in the feet, especially at night
- Loss of sense of touch or sensitivity to touch
- Coordination problems when walking
- Muscle weakness
- Dizziness upon standing
- Decreased or increased sweating
- Digestion issues, such as nausea, indigestion, bloating, vomiting, diarrhea or constipation
- Incomplete emptying of the bladder
- Sexual issues, such as vaginal dryness or erectile dysfunction
- Vision issues or double vision
- Increased heart rate
- Inability to sense low blood sugar
Causes
Diabetic neuropathy is most commonly caused from long-term uncontrolled high blood glucose levels. High blood sugar levels weaken the walls of capillaries (small blood vessels) that supply nutrients and oxygen to the nerves. This reduces the amount of oxygen and nutrients delivered to the nerves, which causes nerve damage. Certain medications used to treat diabetes can also cause a decrease in vitamin B-12 levels in the body, which can lead to neuropathy.
Risk factors
Anyone with diabetes can develop diabetic neuropathy. However, certain factors increase the likelihood of developing the condition. These factors include, but are not limited to, the following:
- Uncontrolled blood sugar increases the risk of various complications of diabetes, especially nerve damage linked to neuropathy.
- A history of diabetes increases the risk of developing diabetic neuropathy. Also, as the time an individual has diabetes progresses, the more likely it is that diabetic neuropathy will develop.
- Kidney disease or damage sends toxins into the blood, which can lead to nerve damage. Because diabetes can damage the kidneys, the risk of diabetic neuropathy increases.
- Being overweight with a body mass index of 25 or greater increases the risk of developing diabetic neuropathy.
- Smoking causes hardening and narrowing of the arteries, which reduces blood flow to the feet and legs. This damages the peripheral nerves and causes issues with wound healing.