Pain
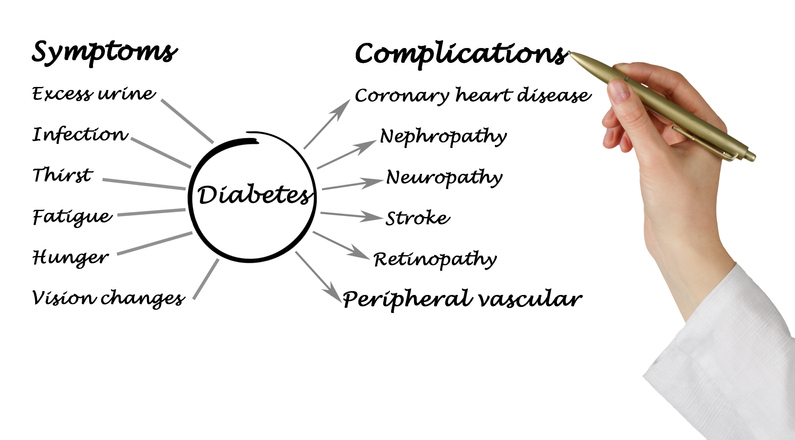
What Is Gestational Diabetes?

Hormonal changes during pregnancy can alter the effectiveness of insulin, resulting in gestational diabetes (a type of diabetes mellitus). During pregnancy, the placenta produces insulin-blocking hormones that cause the body’s cells to become less sensitive to the effects of insulin. This results in high blood sugar levels.
Symptoms of gestational diabetes
In many cases, gestational diabetes does not cause any symptoms. It is typically found during routine blood sugar tests between week 24 and week 28 of gestation. Although rare, symptoms of increased thirst or urination may be experienced.
Causes of gestational diabetes
As the placenta produces hormones to sustain a pregnancy, the body’s cells often become more resistant to insulin. Due to this resistance, the pancreas typically produces extra insulin during pregnancy. If the pancreas is not able to keep up with extra insulin production, glucose remains in the blood instead of going into the body’s cells, resulting in gestational diabetes.
Risk factors for gestational diabetes
Although any pregnant woman can develop gestational diabetes, certain factors increase the risk:
- Overweight before pregnancy or too much weight gain during pregnancy
- Over the age of 25
- A parent or sibling with prediabetes or type 2 diabetes
- Previous delivery of a large baby (over nine pounds) or previous stillbirth delivery
- Black, Hispanic, Native American, or Asian ethnicity
- Certain medical conditions, such as polycystic ovary syndrome (PCOS), high blood pressure, high cholesterol or high triglycerides
It is important to note that a diagnosis of gestational diabetes increases the risk of developing prediabetes or type 2 diabetes following pregnancy.