Pain
Diagnosing Fibromyalgia

What is fibromyalgia?
Fibromyalgia is a chronic pain syndrome that involves widespread muscle pain (myalgias) and joint pain (arthralgias).
Diagnostic process
The diagnostic process for fibromyalgia typically involves a thorough medical history and physical examination. Tests and studies may also be ordered to rule out other health conditions.
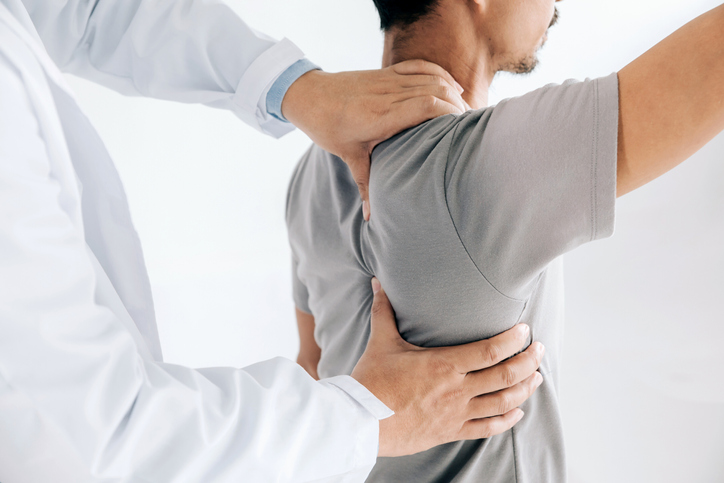
Medical history and physical examination
Clinical clues from a physical exam and medical history that may indicate a fibromyalgia diagnosis include the following:
- Widespread pain that has been present for 3 months or more
- Pain on both the left and right side of the body and above and below the waist
- Widespread Pain Index (WPI)* ≥7 with a Symptom Severity (SS) scale ≥5 OR a WPI of 4-6 with an SS scale ≥ 9
*A WPI quantifies the extent of pain on a scale of 0-19 based on pain or tenderness in 19 different areas of the body. Each tender area is assigned 1 point. The SS scale ranges from 0 to 12 and measures the severity of fatigue (0-3 scale), tiredness upon waking (0-3 scale), and cognitive impairment (0-3 scale). In addition, headaches, lower abdominal pain, and depression are assigned one point each.
Tests and studies
Fibromyalgia is a diagnosis of exclusion, meaning a specific medical test is not available to provide a definitive diagnosis. Other health conditions that cause similar symptoms must be ruled out before a fibromyalgia diagnosis can be made. Medical tests that may be ordered during the diagnostic process include blood and lab tests, imaging studies, and nerve function tests.
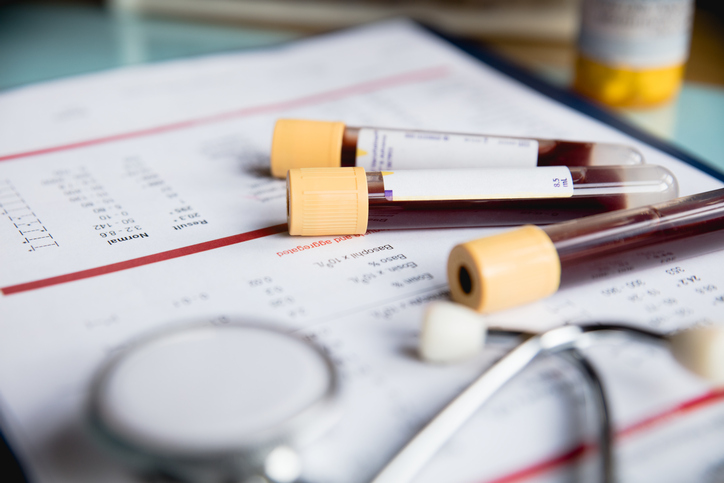
- Blood and lab tests
Certain blood and lab tests may be ordered to rule out other health conditions that cause widespread pain and fatigue. These tests check for the presence of autoantibodies and levels of inflammatory markers to determine if an autoimmune or inflammatory condition is present. Blood tests to check levels of thyroid hormones may also be ordered to make sure the thyroid is functioning properly. A complete blood count and metabolic panel can help identify any kidney or liver issues, anemia, or a chronic infection. - Imaging studies
X-rays, ultrasounds, and MRIs can show any structural issues (e.g., spinal damage, arthritis, etc.) that may be the cause of symptoms. - Electromyography (EMG), nerve conduction study (NCS), or skin biopsy
These tests can help eliminate the possibility that symptoms are caused by neuropathy. A skin biopsy can be used to determine the health of microscopic small fiber nerves. An EMG and NCS can help identify large fiber nerve damage. An EMG involves the insertion of very thin needles into specific muscles to determine nerve and muscle function. An NCS involves the placement of electrodes on different areas of the skin. A low electrical current is used to stimulate the nerve fibers to determine how strongly and quickly the nerves transmit signals. - Potential new tests
Blood tests to definitively diagnose fibromyalgia are currently under development. One test examines plasma and peripheral blood mononuclear cells (PMBC) within blood samples and measures the level of cytokines (inflammatory proteins) in the blood. Abnormally low levels of cytokines may indicate fibromyalgia. Another test under development is an RNA analysis; this test can determine what is occurring within the body's blood cells and has a 94% accuracy rate in the diagnosis of fibromyalgia.